
Weight-Loss Drug Price Cuts Reshape US Pharmaceutical Market Amid Fierce Competition and Shifting Patient Access Strategies
The landscape of prescription drug affordability in the United States is undergoing a significant transformation, particularly within the burgeoning market for weight-loss medications. Driven by intense competition and a unique set of market dynamics, manufacturers of GLP-1 receptor agonists, such as Eli Lilly’s Zepbound and Novo Nordisk’s Wegovy, have begun implementing substantial price reductions, directly impacting the growing segment of self-paying patients. This shift offers a glimpse into how direct-to-consumer sales models might challenge the traditionally opaque US pharmaceutical pricing system, though fundamental questions of universal access persist.
For individuals like Ruth Gonzalez, a 56-year-old self-employed resident, these price adjustments represent a lifeline. When she first sought a prescription for Zepbound last year, the initial monthly cost of roughly $350 (£260) presented a formidable financial hurdle. Her health insurance, like many in the US, explicitly excluded coverage for weight-loss medications. To afford the drug, Gonzalez meticulously re-evaluated her budget, sacrificing streaming subscriptions, adjusting her mobile phone plan, tightening grocery spending, and eliminating discretionary purchases like Starbucks coffee. The sacrifices, she contends, were entirely justified. Within six weeks, her dangerously elevated blood pressure normalized, addressing the primary health concern that prompted her to seek treatment. Beyond that, she achieved a significant weight loss of over 40 pounds (18 kg), bringing her weight down to 175 pounds (79 kg), a change she anticipates will alleviate co-morbid conditions such as sleep apnea and incipient fatty liver disease.
Remarkably, the financial strain on Gonzalez has started to ease due to market shifts. In December, Eli Lilly, the manufacturer of Zepbound, incrementally lowered the price of its vials by $50-$100 (£37.50-£75). This reduction allowed Gonzalez to transition to a more potent, and previously more expensive, dose without increasing her out-of-pocket expenditure. Looking ahead, she is optimistic about further cost reductions, particularly with the anticipated launch of a lower-cost oral weight-loss pill from Eli Lilly in the coming months. "For someone on a fixed budget, it is absolutely helpful," Gonzalez stated, underscoring the tangible benefits of these price adjustments for consumers navigating the complexities of US healthcare costs.
The Unprecedented Dynamics of the GLP-1 Market
The price cuts observed in the GLP-1 segment are particularly noteworthy in the United States, a nation long grappling with some of the highest prescription drug prices globally. This phenomenon is a direct consequence of a confluence of factors, including fierce pharmaceutical competition, the massive scale of the obesity epidemic, and the unusual reluctance of many private and governmental insurers to cover these drugs solely for weight management.
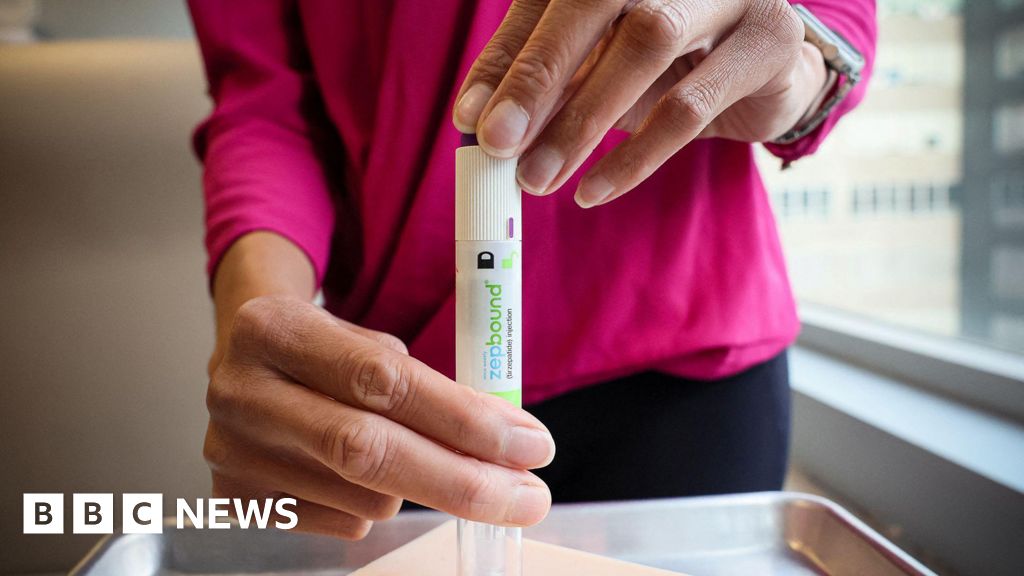
The US faces a significant public health challenge, with approximately 40% of its adult population classified as obese. This condition is a major driver of numerous chronic diseases, including Type 2 diabetes, cardiovascular disease, certain cancers, and musculoskeletal disorders, collectively imposing an enormous economic burden on the healthcare system—estimated to be hundreds of billions of dollars annually in direct and indirect costs. The advent of GLP-1 receptor agonists has been hailed as a breakthrough, offering unprecedented efficacy in weight reduction and improved metabolic health. Originally developed to treat Type 2 diabetes (e.g., Ozempic, Mounjaro), these medications were later approved for chronic weight management (Wegovy, Zepbound) due to their profound impact on appetite regulation and satiety.
The immense market potential—with tens of millions of potential patients—has spurred an aggressive competitive environment. Unlike many other therapeutic areas where new drugs enjoy a period of market dominance, the weight-loss drug sector has quickly become a battleground. This intense rivalry between pharmaceutical giants, primarily Novo Nordisk (Wegovy, Ozempic) and Eli Lilly (Zepbound, Mounjaro), has compelled companies to adopt strategies more akin to consumer product retailers than traditional pharmaceutical firms.
A Chronology of Pricing and Market Evolution
The journey of GLP-1s to their current pricing dynamics can be traced through several key milestones:
- 2017-2022: Diabetes First, Weight Loss Second: Semaglutide (Ozempic) and tirzepatide (Mounjaro) were initially approved for Type 2 diabetes, quickly gaining traction due to their efficacy in both blood sugar control and weight reduction. Their list prices were already substantial, reflecting R&D investments and perceived value.
- June 2021: Wegovy’s Entry: Novo Nordisk received FDA approval for Wegovy (higher dose semaglutide) specifically for chronic weight management. It launched with a list price exceeding $1,600 per month, sparking both excitement and concern over accessibility.
- November 2023: Zepbound’s Debut: Eli Lilly’s Zepbound (higher dose tirzepatide) secured FDA approval for weight loss. Its initial list price was set at over $1,000 per month, entering a market already defined by high costs.
- Late 2023 – Early 2024: The Price War Begins: Faced with sluggish insurance coverage for weight loss and a burgeoning self-pay market, manufacturers began offering significant discounts. A starting dose of Wegovy, which once cost over $1,600, is now available to self-pay patients for as little as $149 a month through manufacturer coupon programs. Similarly, Zepbound’s starting dose has fallen from over $1,000 to around $299 a month for those utilizing discount cards.
These dramatic price reductions are not merely altruistic gestures but a strategic response to market realities. The primary driver is the significant hurdle of insurance coverage. Many major private and government health insurers in the US have "baulked" at the prospect of covering these expensive, long-term medications for millions of patients, citing fears of unsustainable costs. This has created a massive segment of patients, like Ruth Gonzalez, who must pay out-of-pocket, forcing pharmaceutical companies to compete directly for their business.
The Rise of Direct-to-Consumer Models
In response to this unique market environment, pharmaceutical companies have ventured into direct-to-consumer (DTC) sales and distribution channels, a departure from their traditional model of negotiating with pharmacy benefit managers (PBMs) and insurers. This approach includes:
- Manufacturer Websites and Discount Programs: Companies have launched dedicated websites offering savings cards, coupons, and direct purchasing options, often significantly reducing the out-of-pocket cost for uninsured or underinsured patients.
- Retail Partnerships: Strategic alliances with major retailers like Walmart and Costco have emerged, allowing for broader distribution and often leveraging the retailers’ existing pharmacy networks and pricing power to offer more competitive rates.
- Legal Battles Against Off-Label Alternatives: The high demand and initial shortages of GLP-1s led to a proliferation of compounded versions and products sourced from international pharmacies, often at significantly lower prices. Manufacturers have aggressively pursued legal action against these "off-label" rivals, arguing intellectual property infringement and safety concerns, thereby protecting their market share.
This shift has ignited discussions about its potential to disrupt the broader US drug pricing system. Economist Alison Sexton Ward, a senior scholar at the University of Southern California, observes, "What it does is highlight some of the lack of transparency. So… it is pushing this idea of direct-to-consumer." This model bypasses PBMs, which are third-party administrators that negotiate drug prices between manufacturers and health insurance plans, often criticized for their role in the complex and opaque pricing structure that results in high list prices and varying net costs. By going direct, manufacturers expose their pricing more openly, potentially fostering greater competition.
The concept has even gained traction at the policy level. In February, the White House under President Trump launched "TrumpRx," a website designed to connect consumers directly with drug manufacturers for a select group of medications. This initiative aligns with the administration’s broader push for greater price transparency and lower drug costs, echoing the sentiments of drugmakers who have often blamed PBMs for inflating US medicine costs. While pharmaceutical firms have expressed interest in exploring DTC sales for other drug categories, experts remain cautious about the universal applicability of this model. The unique demand and competitive intensity of the GLP-1 market may not translate to other therapeutic areas, where patient populations are smaller and competition less fierce.
Persistent Challenges in Patient Access
Despite the emerging trend of price reductions and direct-to-consumer options, a significant affordability gap persists, leaving many vulnerable patients unable to access these life-changing medications. Shekinah Samayah-Thomas, a 62-year-old resident, embodies this challenge. Having undergone bariatric surgery in 2017 after reaching a weight of 330 pounds (150 kg), she found Wegovy crucial for maintaining her weight loss, which had started to creep back up. However, her access was abruptly cut in January when California’s Medicaid program ceased covering the drug for weight loss.
Samayah-Thomas’s requests for continued coverage, despite a diagnosis of sleep apnea—a condition often improved by weight loss—have been denied. Now, with both she and her husband out of work, even the modest $25 monthly co-pay she once managed through a combination of her husband’s former employer’s insurance and a manufacturer’s coupon is unattainable. "I don’t have it," she laments, highlighting the stark reality that even discounted prices remain out of reach for those with limited financial resources.
Health advocates and patient organizations are thus maintaining their focus on broader systemic solutions. Tracy Zvenyach, Vice President for Advocacy and Research at the Obesity Action Coalition (OAC), emphasizes that while direct-to-consumer options provide a "short-term solution," they must not "deter from the overall goals of general, standard coverage of treatments for obesity." The OAC and similar groups are actively lobbying for obesity to be recognized and treated as a chronic disease by insurers, thereby expanding coverage mandates.

A potentially more impactful development than the DTC trend is the Trump administration’s decision to launch a trial program in July for Medicare to begin covering GLP-1 drugs for specific obesity-related conditions. This move is significant because Medicare, as a major federal health program, often sets precedents that influence private insurers. Should the trial prove successful and lead to broader Medicare coverage, it could significantly sway private payers to expand their own coverage policies, ultimately improving access for millions of Americans.
Broader Implications and Future Outlook
The evolving market for weight-loss drugs presents a fascinating case study in US pharmaceutical pricing and access. While the direct-to-consumer model has demonstrated a capacity to drive down prices in a highly competitive and high-demand segment, experts like Michael Murphy, a professor of clinical pharmacy at Ohio State University, caution that it is not a panacea. "Hopefully this will drive additional consumer awareness of the drivers of the high costs of medication," Murphy stated. But he added, "We need to see further, more fundamental solutions be employed to actually bring down costs overall to the system."
The long-term implications are multi-faceted. As patents eventually expire and more competitors, including those offering lower-priced oral alternatives, enter the market, sustained downward pressure on prices is anticipated. This could lead to a more equitable distribution of these transformative medicines. However, the ethical debate surrounding the "medical necessity" versus "lifestyle drug" perception of weight-loss medications continues to shape insurance coverage decisions.
Ultimately, the GLP-1 market serves as a microcosm of the larger challenges facing the US healthcare system. It highlights the tension between pharmaceutical innovation and affordability, the complex role of intermediaries like PBMs, and the enduring struggle for equitable patient access. While individual stories like Ruth Gonzalez’s offer hope, the experiences of others like Shekinah Samayah-Thomas underscore the urgent need for comprehensive policy changes to ensure that medical breakthroughs are accessible to all who need them, not just those who can afford to pay out of pocket. The coming years will reveal whether the current market disruption is a temporary anomaly or a harbinger of a more transparent and competitive future for drug pricing in the US.



